DOS 523 - Special Topic 1
Writing Prompt
Initial Post: Normal Tissue Complication Probability (NTCP)
"Essentially, all models are wrong, but some are useful."1
George E.P. Box
Normal Tissue Complication Probability, or NTCP, is a statistical tool used when evaluating treatment plans, along with tumor control probability (TCP).2 When physicians make decisions about the amount of radiation dose to prescribe for treatment for a given patient, there are usually a multitude of factors to consider, such as "am I applying enough dose to control the tumor" and "am I applying too much dose for the surrounding tissues to tolerate?" These are often competing goals, because more radiation translates to more destruction of the cancer tissue, but more radiation also translates to more destruction of everything around the tumor. Since two people with identical disease states may respond differently to the same treatment, the only thing that a physician can do to help guide their prescription is to examine a large population of similar patients and compile statistics on their performance when treated with various dose prescriptions. While there may be a wide range of outcomes, it is possible that trends may appear.
Radiation effects on tissue can be categorized as either stochastic or nonstochastic.3 Stochastic effects are ones that are based on probability and are more or less binary in nature; it happens or it doesn't happen. The severity of the result does not change with radiation dose; just the probability that the result will happen. One can think of playing a game of Russian Roulette with a revolver that has a thousand chambers. Increasing dose adds more bullets to the cylinder, but it does not change the fact that if the hammer falls on an empty chamber, nothing bad happens, whereas if it falls on a live bullet, the gun goes off.

Stochastic effects are binary. Image credit: Pete Gardner/Getty Images
Nonstochastic effects are ones that increase in severity as dose increases. This can be a result of more and more cells in an organ dying, further and further impairing its function.
The complication effect that radiation has on the cells of organs and the resulting impairment of the function of the organs can depend on how the organ is organized at a functional level.2 If the organ is examined at the level of functional subunits (FSUs) that cooperate to carry out the function of the organ, two models emerge. A serial organ like the spinal cord that has nerve bundles as its FSU behaves like a chain. If one link in the chain is broken, the entire chain is effectively broken and the organ is unable to carry out its function. Another example of a serial organ is the esophagus. A parallel organ is one that has its FSUs organized to share labor, such as nephrons in the kidney or alveoli of the lung. If some are compromised by radiation damage, the overall function of the organ will be diminished but not destroyed.
There is some parallel between the ideas of stochastic versus non-stochastic and serial versus parallel tissue complications. With a serial organ, probability can be pushed as far as a physician is willing, but if the organ fails, it fails completely. With a parallel organ, the physician may decide that some impairment of the organ is acceptable if it means a higher chance of curing the patient's disease. Walking on thin ice, if ice breaks and the water isn't very deep, maybe you'll just lose a shoe in the mud. You'll be impaired but able to keep going. More dose might correspond to more water depth.

Impaired but still alive. Picture from Izismile.4
A noteworthy fact about parallel organs is that they often have a functional reserve. This means they are able to accomodate bursts of peak usage, but most of the time they are operating below full capacity. This functional reserve can be important to consider when modeling the likelihood of adverse effects, because it means that there is a threshold of dose and damage that can occur before any impairment of normal organ function occurs. Using up the reserve does of course mean that under high demand conditions, the organ will no longer be able to keep up, but high demand conditions may be able to be avoided by modifying patient behaviors after treatment.
Many groups have proposed as many models for predicting both TCP and NTCP. In 1991, Emami et al5 published the results of an extensive literature review aimed at determining the probability of liver toxicity when the liver is uniformly irradiated with full coverage, 2/3 coverage, and 1/3 coverage at various dose levels. Concepts of TD5 and TD50 (the tolerated dose where 5% of the subjects or 50% of the subjects developed complications) were used. By graphing these tolerance doses against percentage of the organ irradiated in each case, a rough set of dose volume histogram (DVH) constraints emerged. It was by no means a complete set of data, but it was an important step towards defining a system for determining the tolerance doses of organs.
Efforts like those by Emami et al have continued, and almost 25 years later, much more data have been collected. Projects like the Quantitative Analysis of Normal Tissue Effects in the Clinic (QUANTEC) have attempted to model the probabilities of complication effects for a variety of organ systems other than the liver.6 In these models, risks of the most common complications are given at various dose levels. These risks often form the basis for physicians' DVH constraints when building a plan prescription.
When a physician makes a choice about a dose level to allow for a given organ coverage, it is not a binary choice of "below this level is safe above it is not", but rather "below this level is the preferred amount of risk, and above it is riskier". Hoffman et al suggest that rigidly defined constraints may not be appropriate in all cases, and the patient's own attitudes towards risk versus reward may be considered in choosing a plan as well.7 Armed with data about probabilities of a cure (TCP) and probabilities of various side effects (NTCP), a range of dose options may be selected appropriate. Looking at a set of probability curves for TCP and NTCP of genitourinary (GU) and gastrointestinal (GI) systems, a range of options between 60 and 80 Gy are presented.
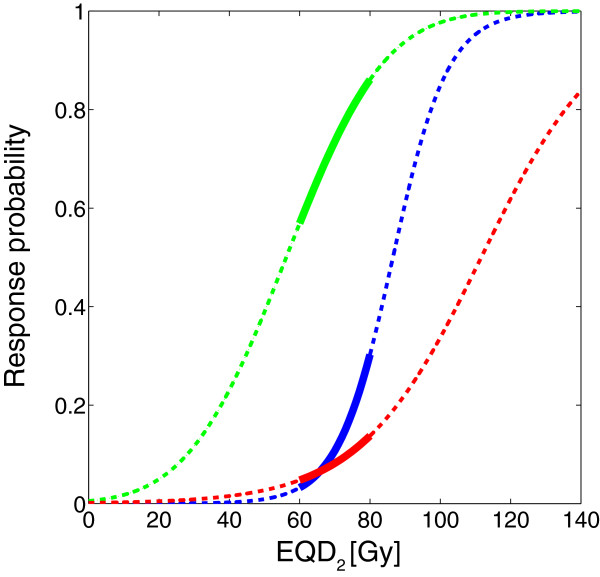
TCP (green), NTCP for GI (blue), NTCP for GU (red)7
At 60 Gy, the risk of GU and GI complications are low but not zero, but the tumor control probability is also low. Jumping up to 80 Gy gives a much better TCP, but the risk of complications also rise. This is a relatively simple representation of NTCP, because it assumes whole organ coverage. For partial coverage of organs such as liver and lung, the chart would have to add the dimension of coverage percentage, which significantly complicates the picture.
NTCP is at the same time a very simple concept and a very complicated concept. There are many factors that influence the probability of outcomes, and many models that predict outcomes in untested ranges. Different organ systems are impaired at different rates, and the severity of the result of their impairment varies as well. Risk can not be avoided, but it can be worked around if the risk is known. Even if no NTCP model is truly accurate, any model is better than just guessing.
Grayden, Chicago
- Box GE, Draper NR. Empirical Model-Building and Response Surfaces. John Wiley & Sons Inc; 1987:424.
- Khan FM, Gerbi BJ. Treatment Planning in Radiation Oncology. 3rd ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2011:443-441.
- Khan FM, Gibbons JP. The Physics of Radiation Therapy. 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2012:351.
- On thin ice. Izismile Website. http://izismile.com/2010/01/13/on_thin_ice_7_pics.html. Published January 13, 2010. Accessed March 29, 2015.
- Emami B, Lyman J, Brown A, Coia L, Goitein M, Munzenrider JE, Shank B, Solin LJ, Wesson M. Int J Radiat Oncol Biol Phys. 1991;21(1):109-22.
- Marks LB, Yorke ED, Jackson A, et al. Use of normal tissue complication probability models in the clinic. Int J Radiat Oncol Biol Phys. 2010;76(3 Suppl):S10-9.
- Hoffmann AL, Huizenga H, Kaanders JH. Employing the therapeutic operating characteristic (TOC) graph for individualised dose prescription. Radiat Oncol. 2013;8:55.
|
Academic Courses > DOS 523 > Normal Tissue Complication Probability (NTCP)
|
Written March 29, 2015
Second Semester, 3 Months into Internship |