DOS 525 - Week 5 Discussion
Writing Prompt
Initial Post: Interstitial Brachytherapy for Base of Tongue
Interstitial brachytherapy, in which the radiation source is inserted directly into a tissue using a surgical procedure, can be an effective method of delivering localized dose to a tumor, either as a primary treatment or as a boost to an external beam plan.1 Recently, I was able to assist with the setup and delivery of a base of tongue boost plan using high dose rate (HDR) brachytherapy with an Ir-192 source.
The patient in question had already undergone a round of external beam photon treatment and a photon boost, so a 3D CT scan already existed, which showed the location of the lesion. From this information, a plan to insert 6 catheters in 2 rows of 3 was developed. Under full anaesthesia, a tracheostomy tube was inserted to allow the patient to breath without disruption due to the apparatus that would be inserted into his mouth. Next, hollow needles were inserted under the chin, through the tumor site in the tongue, and into the air space of the pharynx. Sealed catheters with radiopaque buttons at one terminal end and a thin plastic tail at the other end were inserted tail first by capturing the tail and drawing it back through the hollow needle, pulling the catheter along with it. The catheter was pulled through the needle until the button sat against the surface of the tongue and the tail and excess length of the catheter rested outside the body below the chin. Once each catheter was in place, the needle was removed and a plastic button was threaded onto the outside portion of the catheter and snugged up against the outer skin surface. The two buttons, one inside the mouth and one on the external surface of the neck, held the catheters in place.
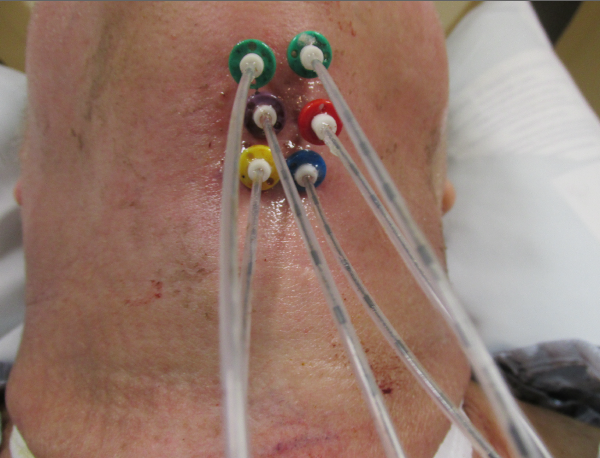
Figure 1. Catheter placement for base of tongue interstitial brachytherapy. Dummy wires with radiopaque markers used for setup verification are visible inside the catheters.
The patient was allowed to recover from surgery, regaining consciousness. Once the catheters were in place, they needed to be prepared for connection to the afterloader machine. This was done under conscious sedation with significant pain medication administered, due to the fresh surgical site and sensitive tissues. Each catheter had a plastic filler wire inside it to provide some stiffness to prevent kinking during implantation and and each was sealed at the tail end to keep the internal surfaces clean and sterile. The outer portion of each catheter was first cleaned of dried blood left over from implantation, and then the ends were clipped just above the transition zone where the catheter narrowed to the tail. The clipper used was designed to only cut the outer sheath and not the plastic core, allowing the tail and a few centimeters of excess catheter to be removed while still leaving enough plastic core to grasp, allowing it to be pulled out, leaving the catheter hollow.
Protocol dictated that the catheters all be trimmed to exactly 20 cm, so that when they were attached to 110 cm transfer tubes, the total length would be 130 cm. A wire with a marking at 20 cm was inserted into each catheter and the catheter was then marked, the wire was removed, and the catheter was clipped. A deburring tool was applied to each clipped end to remove any sharp spurs left over from clipping. Once each catheter was clipped, depth was once again tested with the marked wire, and then a dummy wire with radiopaque markers was inserted into each catheter to help visualize placement on x-ray imaging.
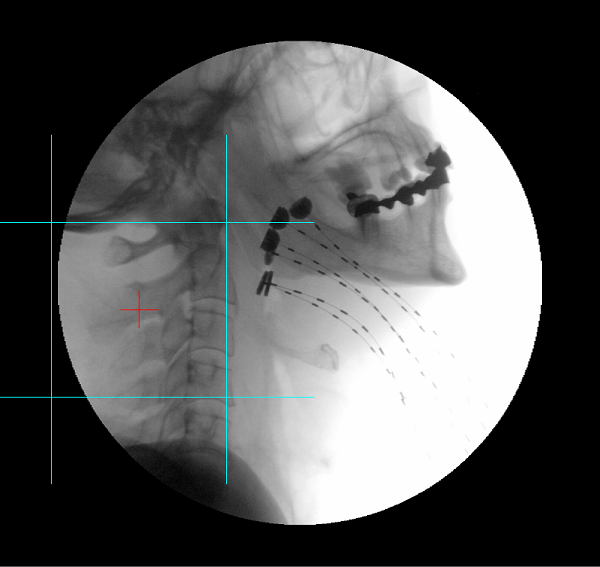
Figure 2. X-ray of dummy wires inserted into interstitial brachytherapy catheters used for base of tongue treatment. Two styles of button are visible because a new style was being evaluated.
The x-ray image was evaluated for straightness of the catheters, regularity of spacing, and whether or not the dummy wires were able to be inserted all the way to the end of each catheter, as indicated by the radiopaque buttons. Once catheter placement was radiographically recorded, the patient was connected to the afterloader for a dummy procedure to test the catheter lengths and integrity. As each transfer tube was connected, it was labeled and then a wire marked at 130 cm was manually threaded into the combination of transfer tube and catheter, feeling for friction, blockages, and then lightly bumping against the catheter end while checking total length. Once each transfer tube was connected to the appropriate catheter and labeled, the other end of all of the transfer tubes was connected to the afterloader. The afterloader was directed to perform its length check QA process, which verified the manual measurements.
Once catheter preparation was complete, the patient was brought to the CT simulator and scanned without any special head restraint. The CT images were brought in to the Brachyvision module of Varian Eclipse, and the plastic catheters showed up as dark channels through the tissue. The channels were defined in software by aligning a virtual source wire to the dark streaks for each catheter channel.
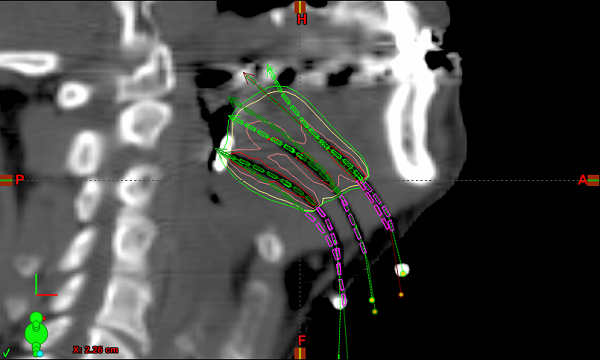
Figure 3. Brachyvision planning for base of tongue interstitial treatment.
The end point of each catheter was established based on the imaging, and the dwell points along each catheter were automatically marked by the software by tracing the path along the channels in 5 mm increments. Dwell times were assigned for each position in order to achieve the desired dose distribution, which in this case was 340 cGy per fraction to the tumor site.
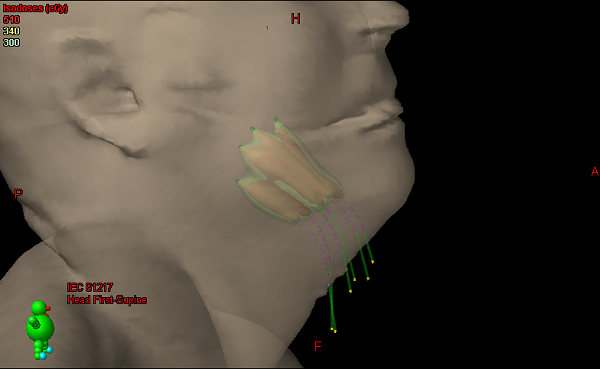
Figure 4. 3D rendering of completed HDR base of tongue boost plan
The delivery process involved connecting the transfer tubes to the catheters and then to the afterloader. Lengths were once again verified both manually by manually threading in a 130 cm marked wire, and by running a computerized length verification routine using a dummy wire contained in the afterloader unit. Once the setup was confirmed, the afterloader extended the source to the end of each catheter, dwelled for a specified amount of time, and then stepped back in 5 mm increments, dwelling at each point for the appropriate amount of time. This was done for each catheter. Total treatment time for all six catheters was under 2 minutes, the vast majority of total procedure time was setup and quality assurance. The patient's whole boost treatment consisted of 4 treatments, delivered twice per day (morning and late afternoon) for 2 days.
After all of the treatments were delivered, the catheters were removed by pulling them back out through the mouth, the way they came in. The alternative was to clip the buttons off the inside end of the catheters, but this was considered to be too high of a choking hazard. The tracheostomy tube was also removed at this time.
Grayden, Chicago
- Bentel GC. Radiation Therapy Planning. 2nd ed. New York, NY: McGraw Hill; 1992.
|
Academic Courses > DOS 525 > Interstitial Brachytherapy for Base of Tongue
|
Written May 6, 2015
Second Semester, 4 Months into Internship |