DOS 525 - Week 3 Discussion
Writing Prompt
Initial Post: COMS Eye Plaque Brachytherapy
Melanoma of the choroid of the eye is a rare disease,1 but it is the most common malignant ocular tumor in adults.2 The most common therapy for this disease is removal of the affected eye (enucleation), but radiation therapy is also an option for treatment. Because of the sensitive nature of nearby tissues, low energy radiation with a short range is preferable, and one technique that has evolved over the years is the use of brachytherapy eye plaques. These devices are built to serve as a caddy for radioactive materials, usually encased in small sealed metal tubes that resemble grains of rice. These seeds are arranged inside the concave surface of the plaque, and the plaque is surgically attached to the eye over the site of the tumor for a short course of brachytherapy (Figure 1).
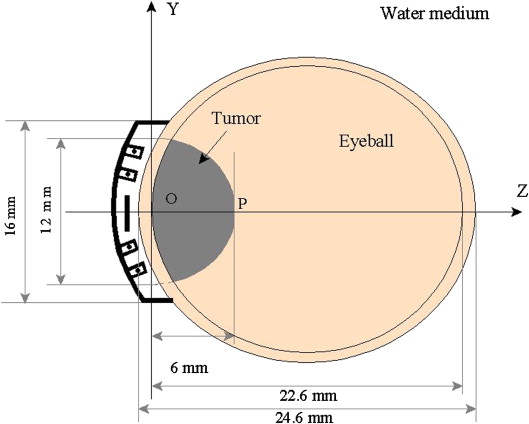
Figure 1. Schematic of an idealized placement of a COMS plaque in a phantom study.3
In 1986, a multicenter clinical trial called the Collaborative Ocular Melanoma Study (COMS) Medium Tumor Trial was initiated with the goal of determining whether enucleation or eye plaque brachytherapy had better long term survival outcomes.1 Patients were randomized, with some patients undergoing enucleation, and some receiving a 5 day course of brachytherapy with eye plaques. In order to standardize the study, the COMS group created a standard design that all centers would use. The original study included 5 standard sizes ranging from 12-20 mm in 2mm increments, although the same basic design is now available in 7 standardized sizes ranging from 10-22 mm.3 The construction of a COMS plaque consists of a concave gold alloy backing with a short cylindrical rim featuring loops for sutures. Inside the dish formed by the gold backing is a layer of a polymer material called silastic withcutouts to hold the seeds in a specific array layout. Seeds containing 125I are loaded into the plaque and the plaque is then sutured to the eye (Figure 2).
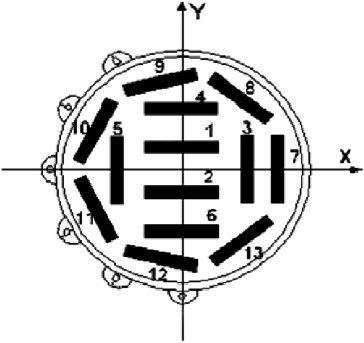
Figure 2. Schematic of 125I seed layout inside a COMS plaque.3
The initial data was inconclusive, with no statistical difference in the 5 year survival between the two groups.2 Krintz et al have highlighted some potential shortcomings in the design of the original trial, which made several simplifying assumptions including treating the seeds as point sources with no corrections for anisotropy, attenuation from the rim of the plaque, backscatter from the gold backing, or attenuation by the silastic insert. The silastic material has a high silicon content around of around 40% by weight, so its effective atomic number is around 11, giving it an attenuation coefficient about 2.2 times higher than water for 125I photons. Once the data was reexamined with these corrections included, doses to structures of interest may have been miscalculated, resulting in doses from 7-21% below what was expected.
Eye plaques are not used at my clinical site. Other forms of ocular melanoma treatment with radiation are available, including a new ocular melanoma proton program at SCCA Proton Therapy. If radiation can prevent the removal of an eye and preserve function, that seems to me to be a better option than enucleation.
Grayden, Chicago
- Design and methods of a clinical trial for a rare condition: the Collaborative Ocular Melanoma Study. COMS Report No. 3. Control Clin Trials. 1993;14(5):362-91. http://dx.doi.org/10.1016/0197-2456(93)90052-F
- Krintz AL, Hanson WF, Ibbott GS, Followill DS. A reanalysis of the Collaborative Ocular Melanoma Study Medium Tumor Trial eye plaque dosimetry. Int J Radiat Oncol Biol Phys. 2003;56(3):889-98. http://dx.doi.org/10.1016/S0360-3016(03)00211-6
- Zhang H, Martin D, Chiu-tsao ST, Meigooni A, Thomadsen BR. A comprehensive dosimetric comparison between (131)Cs and (125)I brachytherapy sources for COMS eye plaque implant. Brachytherapy. 2010;9(4):362-72. http://dx.doi.org/10.1016/j.brachy.2009.07.007
|
Academic Courses > DOS 525 > COMS Eye Plaque Brachytherapy
|
Written April 22, 2015
Second Semester, 4 Months into Internship |