DOS 511 - Week 1 Discussion
Writing Prompt
Digital imaging seems to be taking over in radiation therapy. What are the primary benefits to digital imaging and do you see any advantage in not completely converting to digital imaging?
Initial Post: Advantages of Digital Imaging
Digital imaging has several key advantages over film-based imaging, including rapid processing, a characteristic curve that is linear over a wide exposure range1, the ability to be copied, shared, and viewed simultaneously by several users on several kinds of devices2, the ability to be post-processed to perform special analyses, and the ability to include store 3-dimensional or even 4-dimensional (3D plus time) data.
Film-based imaging must accurately calculate the correct exposure time up front in order to produce a film that appropriately visualizes the desired range of densities within the useful range of optical densities provided by the film. Digitally acquired images such as CTs can capture thousands of distinct intensity levels simultaneously. This is far more than the human eye can perceive at once, and more than most display devices can display as well. Details that are lost in the shadows or washed out in the highlights can be brought into a viewable range simply by adjusting the black point and white point of an image set so that a grayscale is mapped across a desired range of values. Here is a series of images that are all the same slice of the same CT, but with different sections of the contrast range highlighted, as seen in the histogram overlaid onto each one:
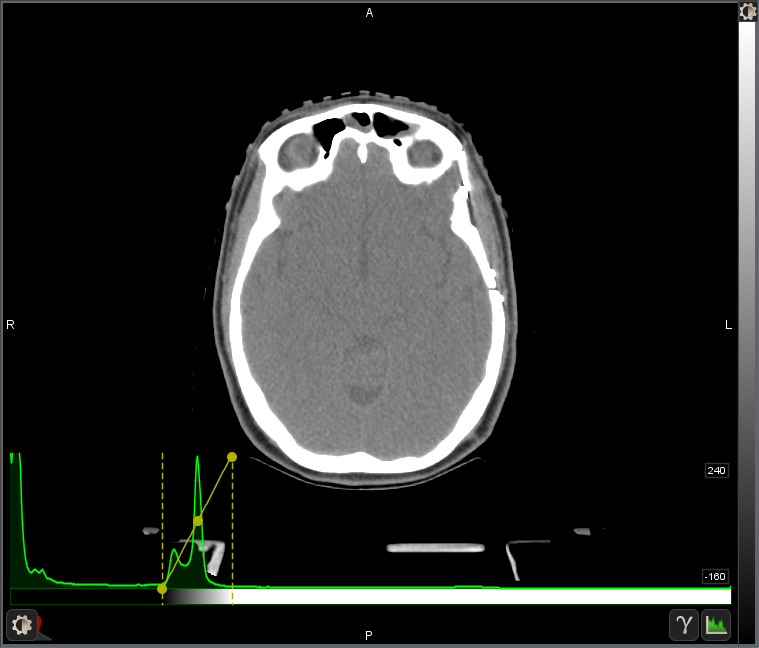
Here is a CT of the head in a standard "soft tissue" contrast setting with black set at -160 HU (near the air/tissue boundary) and white set at 240 HU (low density bone). This makes anything less dense than tissue (most of the plastic immobilization mask, most of the carbon fiber table, and air) get lost as black pixels, and anything more dense than low density bone (high density bone, metal) gets washed out as all appearing white. The yellow bounding lines on the green histogram show which portion of the full range of intensities will be rendered in grayscale, with anything to the left as pure black and anything to the right as pure white.
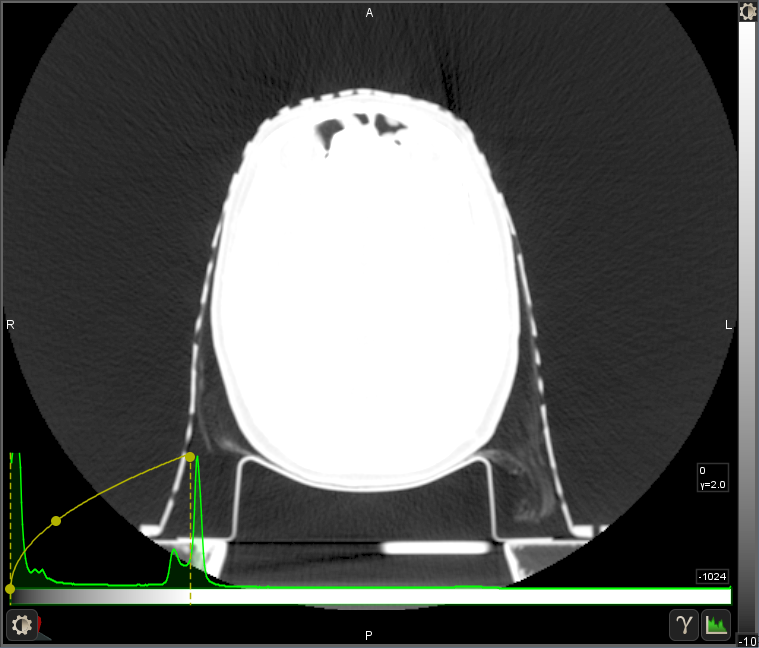
Here is the same image with black set at -1024 HU (air) and white set at 0 HU (water), with a gamma correction of 2.0 which biases the curve to bring out details in the dark end. This completely loses the detail of the patient, but it brings out the details of the table, mask, and even hair. I use this setting when contouring the objects surrounding the patient, which is important in proton therapy.
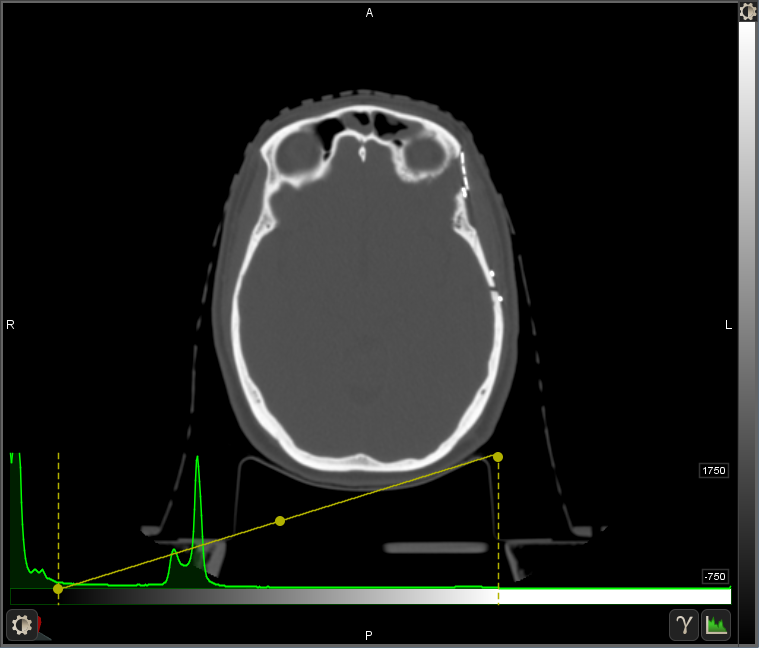
Here again is the same image but this time with a wide window skewed towards higher densities. This makes the differences in bone density and the presence of metal more apparent to the viewer. The metal is near the patient's left eye (one the viewer's right side) and on either side of a cut in the bone on the side of the skull. It is still possible to see where soft tissue is, but all detail except a layer of fat under the skin is lost.
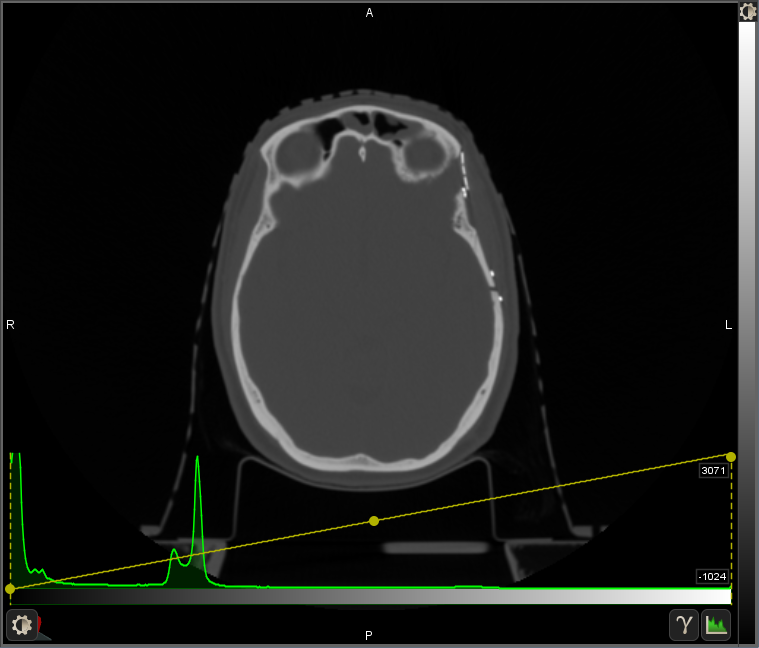
Here's the full range of intensities in one view. Some dynamic range in the bone is lost, and you can just barely start to see some of the hair pinched between the patient's head and the headrest because we are including low values again. By trying to do everything, it excels at nothing.
The CT slices above, which are part of a stack of images covering the head and neck, can be reprocessed to show a sort of projection view from a different angle. Here is a Maximum Intensity Projection (MIP) view, which is somewhat like a standard x-ray, except that instead of adding up the values of all the pixels in a stack, it selects the single brightest pixel in each stack and brings it forward.
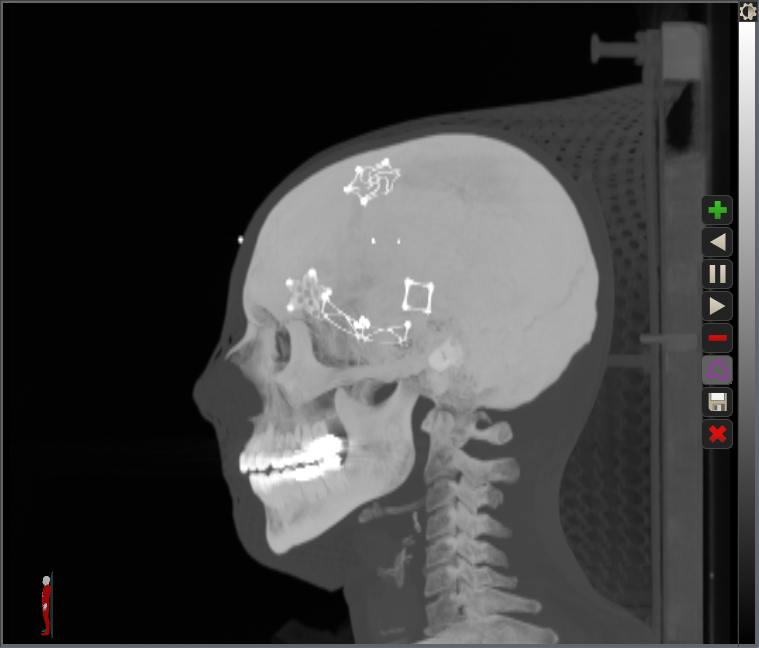
Here it is again but with the window/level adjusted to knock out most of the table and soft tissue.
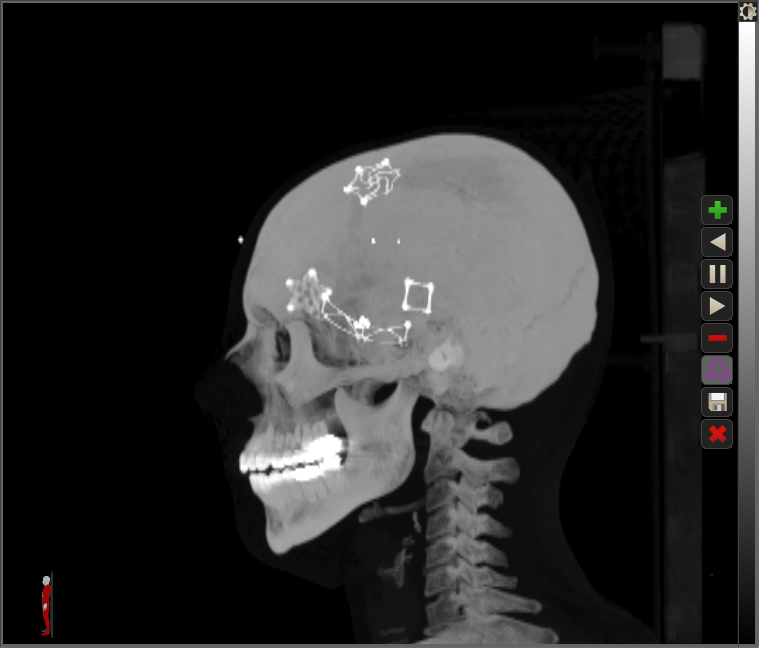
For reference, the star-shaped patterns are pieces of metal called burr hole covers, which span across drill holes from brain surgery, and the square and curvy rectangular pieces are reinforcements to hold a piece of bone that was temporarily moved out of the way during surgery and then put back in place.
These images can be easily shared with other viewers, as we see here. Viewer with access to the full dataset could adjust window/level on their own to get whatever effect they want, and they could explore the entire 3D dataset. If this were a study of the lungs, a 4D image could be obtained that would allow examination of how the 3D anatomy moves during respiratory motion.
These images are not particularly high-resolution (they are only 512x512 pixels), but 2D digital images can go to much higher resolutions (I have seen 4000x3000 and I suspect they can go much higher). I anticipate that film-based imaging will be relegated to special-purpose applications as digital technology continues to improve and come down in price, much as has happened in the world of regular photography.
Grayden, Seattle
- Fleckenstein P, Tranum-Jensen J. Anatomy in Diagnostic Imaging. W B Saunders Company; 2001.
- Washington CM, Leaver DT. Principles and Practice of Radiation Therapy. Mosby; 2010.
Followup Post Directed to Another Student
Maggie,
This is all done in MIM.
Adding gamma to the contrast curve changes the black to white progression from linear to non-linear. In the case of the second image on my original post, it lets me have more of the useful grayscale change happen in the really low densities while not completely washing out everything above. A lot of it still gets washed out, but not as badly as it would have with a linear progression. I only started playing with gamma recently, so I'm still blundering my way through it, and the process of trying to explain it is actually helping me understand it better myself. :-)
I initially misread your question and didn't realize it was all about gamma, so I had made a series of pics to explain how black point and white point affect the image. I might as well post them, since I think they are still useful for that. They are kind of thrown together quickly, so let me know if anything needs to be explained better.
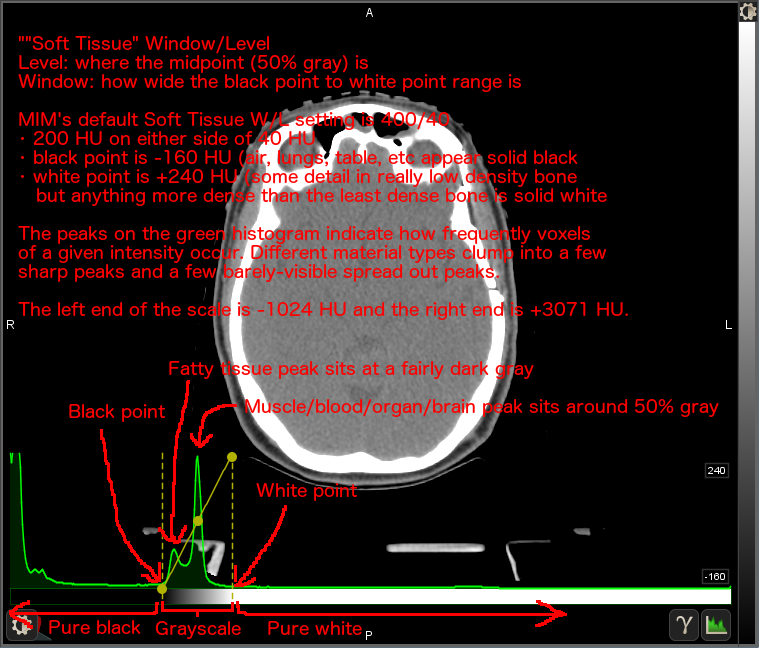
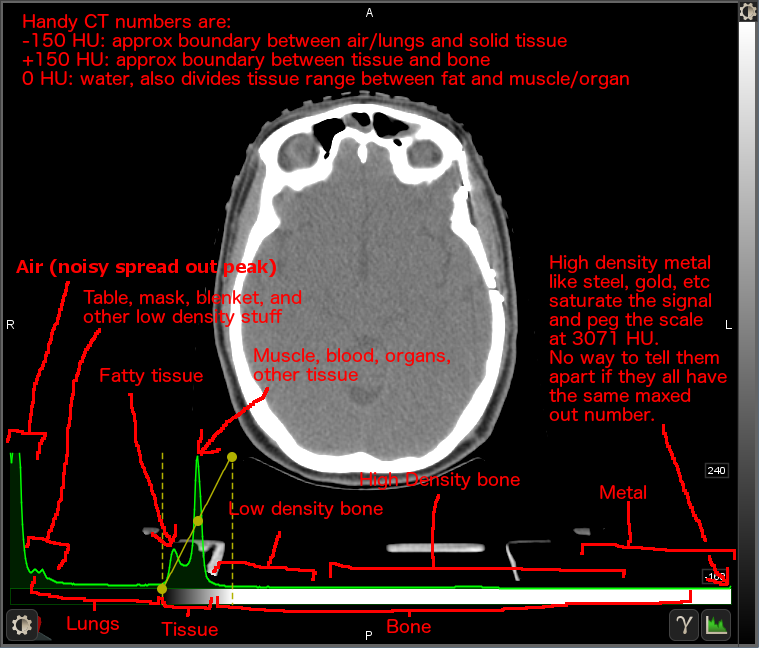
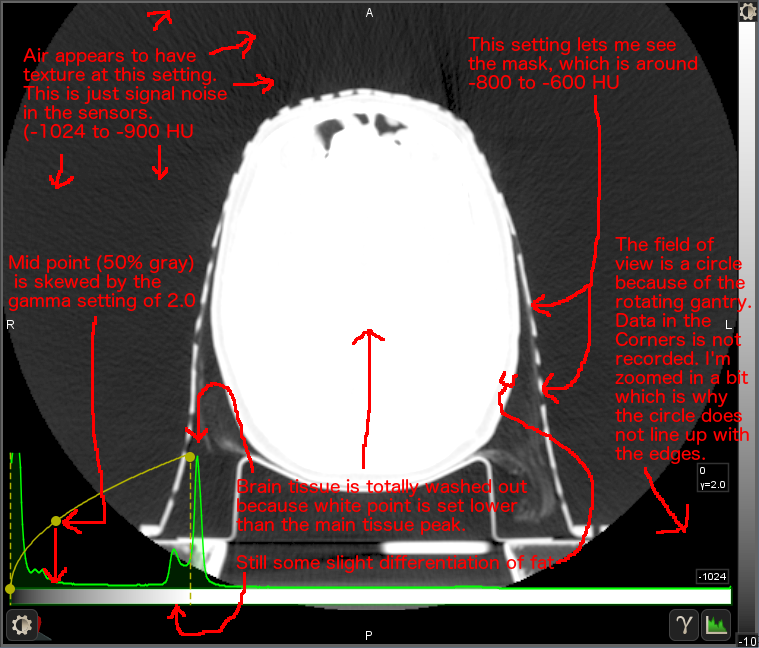
Note: my super-professional-looking arrows were not done in MIM; those are from Gimp. :-)
The option to flatten an image was not actually developed for CT imaging. The concept was developed for PET and SPECT scans, which are mostly empty space with a few interesting blips. By projecting the hot spots forwards and viewing it from multiple angles, you can get a sense of where PET hot spots in a patient are located. In MIM, you would be able to click on a hot spot in the rotating view and it would take you to that spot on the regular slice-view. Here's an example of a rotating PET MIP view:

This patient has a giant tumor in their right lung, and a few PET-avid lymph nodes in their mediastinum. The other high intensity bits are the brain, left ventricle of the heart, liver, kidneys, ureters, and bladder
I tried applying the MIP view idea to a CT instead of a PET and I found that it can be very handy for finding metal in a patient and for understanding the positioning of arms, curvatures of the spine, or other problems with bone or patient positioning. The pic I posted was just one angle of a rotatable view, which is why the image has play and pause buttons.
Grayden, Seattle
|
Academic Courses > DOS 511 > Advantages of Digital Imaging
|
Written November 5, 2014
First Semester, Pre-Internship |